Vaginal Problems: Pelvic Organ Prolapse
Gill Brook, an independent pelvic floor and women's health physiotherapist.
Something's coming down!
At some point in their life many women will experience a prolapse or - to give it its correct name - a pelvic organ prolapse (POP). Some studies suggest that more than 9 out of 10 of us have a degree of prolapse. However many women are not aware of it and, in its mildest form, it might even be considered normal, especially in women who have given birth at some point in their life.
POP is a bulge of one (or more) of the pelvic organs into the vagina. Age is a risk factor; basically the older we get, the more likely we are to have one! Pregnancy and childbirth are other considerations, and research suggests there are some racial and hereditary influences. For instance, you may be more prone to prolapse if a close female relative such as your mother or sister has experienced one. There may also be a link with gynaecological surgery, including hysterectomy. Other risk factors include obesity, smoking, chronic constipation, heavy lifting and pelvic floor muscle weakness.
Possibly a quarter of all women who have a degree of POP will experience symptoms. Typically they describe a feeling of ‘something coming down’ or of heaviness or pressure in the vagina which may be there all the time, or just now and then. It can feel like a tampon that has slipped out of place. Many women can feel something when they are drying themselves after a shower, or – if they check with a mirror – can see a bulge at the mouth of the vagina. This can be worrying for some, who see what they think is a lump or growth, rather than something that has just moved out of place. In addition to the feeling of bulging, etc., there may also be bladder or bowel symptoms, or it can affect a woman’s sex life. You would think that the greater the prolapse the more significant the symptoms and this may be the case, but definitely not always. Some women are aware of a bulge down below, but it causes them no problems at all.
If you do have symptoms then the first port of call is normally your GP or practice nurse who will probably want to examine you to confirm the diagnosis. Depending on what they find, and how much the symptoms are troubling you, there are several possible courses of action. Some women – reassured that it is ‘just’ a prolapse – are happy to continue as they are. Many GPs and practice nurses can offer you appropriate advice, or may refer you to a more specialist healthcare professional such as a women’s health physiotherapist or gynaecologist.
Although there are things that you can’t change – such as your age! – there are others that you can address, and such changes should reduce your symptoms or decrease the risk of them getting worse. For instance, if you are overweight could you reduce this, and improve your diet to help with your bowel function if you suffer from constipation? Can you stop smoking? Look at your heavy lifting; could you reduce this? Either share the load with someone else or (when possible) split it into smaller amounts.
Recent research has proved that pelvic floor muscle exercises can reduce symptoms of a prolapse in many women, and your GP or practice nurse will almost certainly advise you to start these. By the time women have reached the menopause most will have heard of their pelvic floor muscles, but how many know exactly where they are, what they do and - most important of all - how to exercise them correctly and effectively?
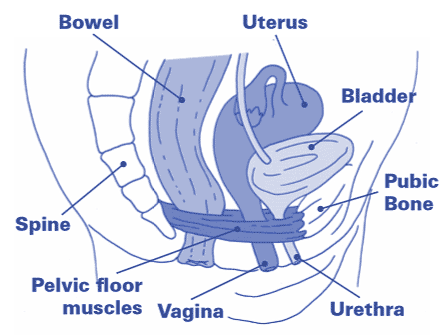 As the name suggests, these essential muscles form the floor of your pelvis, extending from the pubic bone at the front through to your coccyx (tailbone) at the back.
As the name suggests, these essential muscles form the floor of your pelvis, extending from the pubic bone at the front through to your coccyx (tailbone) at the back.
In a nutshell, the pelvic floor muscles have three main functions; they help prevent leakage from your bladder or bowels, contribute to the comfort – and your enjoyment - of sex, and hold your pelvic organs up in place. There is no doubting their importance!
Some women first notice symptoms associated with pelvic floor muscle weakness around the time of the menopause; probably related to the hormonal changes taking place. A large study of perimenopausal women showed that over half experienced some urinary incontinence, and 25% of them wore protection or had to change their underwear regularly because of this.
Pelvic floor muscle exercises
It is really important that you ‘find’ the right muscles to squeeze. Unlike almost every other muscle in your body, they are not visible on the outside so it is easy to get it wrong. You can exercise your pelvic floor muscles in any position, but to start with you may want to sit or lie, comfortable and relaxed, so you can concentrate on what you are doing and feeling.
Squeeze and pull in the muscles around your back passage, as if you are trying to stop yourself from breaking wind. Now also squeeze and lift at the front, as if you are sitting on the toilet trying to stop yourself while passing urine. Hold for a couple of seconds, then let go. Repeat a few times, to get the feel of it.
This is how to squeeze your pelvic floor muscles. If you are not sure that you’re doing it right, then you could check by holding a hand mirror so you can see what’s happening. If you are squeezing the right muscles, then you should see the vaginal opening, anus, and the area between them (the perineum) draw in, away from the mirror. Alternatively, put a finger or two in your vagina, and when you squeeze the muscles you should feel some pressure, even if it is just a little. If you are still not sure, then your GP or practice nurse should be able to examine you to check.
When you squeeze your pelvic floor muscles, you may find that you also pull in your lower abdomen (between your belly button and pubic bone) slightly. This is OK, but you should not be tightening any other muscles.
It may be useful to practise some slow pelvic floor muscle exercises and some fast ones; like you might vary exercises you do at the gym.
First squeeze and lift the muscles slowly and firmly, and hold for as long as you can, up to 10 seconds. Let go, and relax the muscles for a few seconds. Don’t worry if you can only manage a short squeeze - perhaps just a couple of seconds. Start with this, and gradually increase the length of hold as you feel your muscles getting stronger. See if you can do 10 of these slow squeezes, but start with fewer if your muscles tire quickly.
Next squeeze and lift the muscles hard and fast, and let go straight away. Again, see if you can manage 10, or start with fewer.
When you do these exercises, it will only take you a few minutes. No-one is sure exactly how often you should do them, but aim for about 3 times a day. You can do them in any position, which makes them more convenient than a lot of exercises, and nobody can see what you’re doing. The challenge is remembering to do your exercises. Many women now set a reminder in their mobile phone, or download an App; there are several available.
If you are experiencing any symptoms of a POP (or you have been told that you have one) then learn to use your pelvic floor muscles to reduce downward pressure. For example, squeeze and hold the muscles when you are lifting, coughing, sneezing, squatting down or bending over. This should also help if you leak urine at these times.
Pelvic floor muscle training can take 4 months or more to be effective but be patient and persevere; it’s worth it!
Frequently asked questions
Q. I know I have a prolapse as the nurse mentioned it when I had my last smear, but it doesn’t bother me. Should I do something about it?
A. It sounds like you are one of the many women (probably the majority) who have a prolapse but no symptoms. There is probably no need to see a specialist about this unless it becomes a problem. However, there may be some factors you could consider. Are you a healthy weight? If you smoke, could you stop or reduce this? Do you follow a good diet with adequate fibre and fluid intake, and avoid constipation? Also, it would be good to practise pelvic floor muscle exercises to minimise the risk of your POP getting any worse.
--
Q. I have a prolapse, and the doctor has told me that it is the back wall of my vagina and rectum. It is only a problem when I empty my bowels, and I feel that I don’t empty fully. I am practising pelvic floor exercises, but is there anything else I can do?
A. Some women find that it helps if they support the area when they are on the toilet, either by pressing upwards on the area between the vagina and anus (the perineum), or by supporting the back wall of the vagina with a finger or thumb. Whether or not you try this, make sure you don’t strain on the toilet as it could make things worse eventually.
--
Q. I’ve had a hysterectomy so I can’t have a prolapse, can I?
A. Yes, you can. The vagina, bowel or bladder can still prolapse. In fact, research suggests that you might be more at risk of POP after a hysterectomy. So, all the advice and pelvic floor muscle exercises are just as important for you, if not more so.
Other resources
NHS information on pelvic organ prolapse
--
Gill Brook is an independent pelvic floor and women's health physiotherapist in West Yorkshire. In addition to clinical work she teaches, lectures and writes on the subject and is currently secretary of the International Organization of Physical Therapists in Women's Health.
