Osteoporosis
The most important long-term effect of reduced estrogen involves the effects on the skeleton. With age and reduced estrogen levels, particularly when the menopause occurs before the age of 45, there is an increased risk of progressive loss of bone strength leading to bone thinning and fragility (osteoporosis). Bone loss affects both men and women as they age but the loss occurs much more rapidly in women so that osteoporosis is much commoner in women than men.
If you have had an early menopause, it is recommended that hormone therapy is taken at least until the average age of the menopause (early 50s) even if you are not having menopausal symptoms. Hormone therapy in this situation provides significant benefits for bone health, reducing the risk of osteoporosis and fracture. If your early menopause was some years ago and you did not take hormone therapy, it is worth discussing with your doctor or nurse; assessments can be carried out and effective treatments are available if you have bone thinning.
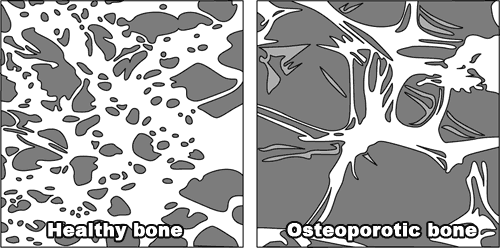
Osteoporosis is defined as: a systemic skeletal disease characterised by low bone mass and microarchitectural deterioraton of bone tissue, with a consequent increase in bone fragility and susceptibility to fracture.
Bone loss itself does not cause any symptoms until a fracture occurs, often as a result of a simple fall. Fractures commonly occur in the wrist, spine and hip. Such fractures can significantly reduce quality of life, independence and, in the case of hip fracture, can shorten life. It has recently been estimated that by the age of 70, one in two of all women and one in five men will have had a fracture related to osteoporosis and that the number of hip fractures worldwide will increase further in the future. Development of osteoporosis in women is influenced by the strength of the bones before the menopause (peak bone mass being achieved in the twenties and being influenced by weight bearing exercise, diet adequate in calcium and vitamin D and by genetic influences), the age of menopause and the rate of bone loss with menopause and age.
Fracture Risk Assessment Tools
FRAX: Calculate your ten year probability of fracture with Bone Mineral Density
https://www.shef.ac.uk/FRAX/tool.jsp
Q Fracture: Calculator to work out your risk of developing any osteoporotic fracture
http://www.qfracture.org
See also
The Royal Osteoporosis Society has launched a new set of online videos and guides ranging from how exercise helps with osteoporosis and bone health, answering common questions, through to specific exercises to promote bone and muscle strength, balance, back pain after a spinal fracture, help with posture, moving and lifting safely, bending forward and Pilates.
Videos and guides are available at: theros.org.uk/information-and-support/osteoporosis.
See also: How HRT can be used as an osteoporosis drug treatment to strengthen bones. (Youtube)
Menopause Matters Magazine article:
Why it's important to look after your bones.

